Complete Guide to Medical Billing and Coding Software
When it comes to medical billing, cashflow and efficiency, the most important decision facing clinics is the selection of the right medical billing and coding software.

Billing medical claims (or physical therapy claims) is an intricate and complex process, even for individuals trained in medical billing and coding. The options are limitless, and pouring through countless online articles (and books) on the best software for medical billing is arduous and time consuming.
That’s why we’ve put together this Complete Guide to Medical Billing and Coding Software, outlining the most critical areas to look for in medical billing and coding software.
Total Integration & Precise Revenue Cycle Management
In 21st century health care, a precise ecosystem in which your key components work together to transmit information is vital to success.
Integration is no longer a matter of convenience – it is a matter of survival.
Your medical billing is dependent upon a wide variety of factors (payer type, secondary and even tertiary insurance, authorizations, eligibility, and more), all of which should be automatically assigned correctly to a claim, ready to be scrubbed and submitted to a clearinghouse.
Medical billing and coding software should be directly connected to eligibility information, the practice’s scheduling component, and an ERA interface.
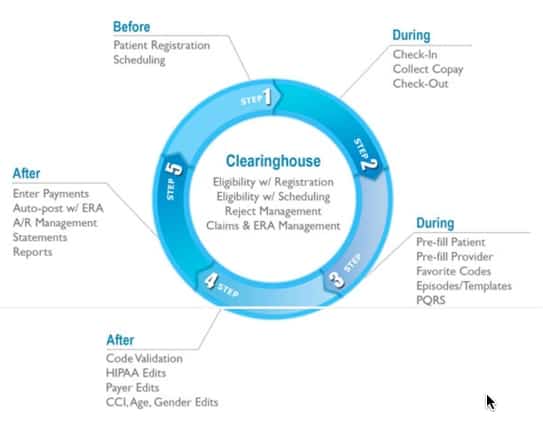
The best possible workflow for a practice should be a simple cycle that analyzes required data points, then populates it where applicable at every step of a patient encounter. Below is a comprehensive breakdown of the most efficient workflow:
- The patient’s eligibility is checked
- Their chart is created with insurance verified information
- Their schedule is set, assigned to a provider and has a custom appointment type for easy tracking
- An ONC Certified medical billing software populates the appointment
- The provider completes the visit and documentation
- Completed note populates as a claim
- Claim populates the information from the eligibility check, from documentation, and from a built in custom fee schedule
- Biller and coder then have an easier and faster experience in scrubbing the claim using integrated scrubbing tools
- Claim is submitted via a built-in clearinghouse component
- Any follow ups are tracked in real-time within the software
- The claim is accepted and returned directly through the software in an on-board ERA dashboard for posting.
Using this method, practices can streamline the entire work flow of the patient encounter by having eligibility, chart creation, scheduling, documentation, fee schedules, pre-scrubbing, clearinghouse submissions, and ERA posting integrated into one systematic methodology.
One-Click Eligibility Status & Instant Patient Chart Creation
All practice’s should have software capable of running instant eligibility checks. This will help the practice determine what a patient’s insurance company will cover, how many visits a patient is entitled to, copay amounts, as well as a plethora of other useful information.
This functionality should be directly connected to your medical coding and billing software interface. When possible, eligibility, scheduling, and chart creation should all happen from within the same program that billing medical claims happens in.
 When these two components are locked into the same system as billing and coding, a distinct advantage occurs.
When these two components are locked into the same system as billing and coding, a distinct advantage occurs.
Once eligibility has been run, front desk personnel should have the capability to create a new or updated patient chart based upon the information and demographics found in the eligibility results. This not only saves the front desk time on entering demographics manually, but when integrated with billing and coding components also ensures that demographics found on the electronic claim form never vary from what is on file with the payer.
This means fewer denials due to typographical errors or due to patients updating information with either the clinic or the insurance company, but not both.
Built-In Clearinghouse Components & Autoposted ERAs
 When a practice owner or clinical manager is about to compare medical billing software from one with another, clearinghouse integration is an important consideration. A completely integrated solution involves real-time, automatic syncing between the EMR software, billing software and clearing house.
When a practice owner or clinical manager is about to compare medical billing software from one with another, clearinghouse integration is an important consideration. A completely integrated solution involves real-time, automatic syncing between the EMR software, billing software and clearing house.
A biller should have the option to track the journey of each claim, from submission to payer status all the way to adjudication.
The biller should be able to get information instantly, without having to call the clearinghouse or payer, and all relevant information should be displayed in an intuitive fashion within the same software. Billing staff should have the ability to easily track claims by payer, patient, provider, date, and monetary amount (down to the penny), at every step of the claim life-cycle.
Should a claim be rejected at the clearinghouse level, the information on the rejection should be displayed within the billing and coding software and adjustments should be easily made and tracked with time-stamped internal notes.
Once a claim is accepted and set for payment, Electronic Remittance Advice (ERA) information should always be populated automatically through the same billing software as a claim was submitted through.
This ensures outstanding claim data is easily compared and contrasted with paid claim data, and leads to a verifiable AR stream.
Billers should be capable of posting ERAs line by line or by batch, which automatically assigns correct dollar values against correctly itemized payment lines.
AR should be a measurable metric, available at the click of a button.
Time-Stamped Internal Notations & Compliance/Pre-Scrubbing Tools.
Even with the best possible systems and software in place, payers will find a way to delay or deny claims. When this happens, it is imperative that billers have a tracking utility built into the same system that a claim was processed through.
Each individual claim should have an area for time-stamped notations, filed by username, to properly identify who is working a claim, the status of the claim, any follow ups or reference numbers for calls with payers, etc. This makes tracking claim submission and resubmits easy and increases reimbursement. The power of payers is in the complexity of the process – simplifying this gives the power back to the biller.
Medical billing software should also include tools for pre-scrubbing claims prior to submission. Using algorithms to find coding discrepancies, missing modifiers, or missing diagnosis pointers will increase first pass rates (ratio of claims being accepted and paid on their first submission) dramatically.
Automated Modifier Rules and Fee Schedules
An important automation trigger that, surprisingly, is yet to become standard in billing and coding software, Modifier Rules and Fee Schedules are time-consuming aspects of billing. These should easily be set up during the implementation phase of a new software, then easily left to work in the background.
Clinicians aren’t billers or coders, and when documentation is finished and populates to billing software as a claim, modifiers should automatically populate based upon pre-programmed rules that billing staff decides upon.
This same methodology should be applied to fee schedules. Since various insurance companies pay out different amounts per code, patients assigned to a specific payer should have the payer-based fee schedule automatically populate for all of their claims without the billing and coding specialist ever having to lift a finger.
Conclusion… and Your Next Step
When the time comes to compare medical billing software solutions, always remember the key components any medical billing and coding software needs have.
Billing medical claims is complex, and there are countless ways for insurance companies to deny clinics money they are rightfully owed.
For more information on how In Touch EMR can simplify your scheduling, documentation, and billing, schedule a demo with us today.
In Touch Biller Pro is a medical billing and coding software with unlimited support via phone, email and live chat, along with a 60 day money back guarantee.
Click here to schedule a free ‘strategy’ call with the experts at In Touch Biller Pro, or call (800)-421-8442 to learn more.
To watch a quick 10 minute overview of In Touch Biller Pro, watch this video below:
Need More Information about In Touch EMR? Contact Us
In Touch EMR is a fully integrated scheduling, documentation and billing software for physical therapy practices. It is a simple and user friendly web-based, ICD-10 and HIPAA compliant EMR, and it offers customizable templates for notes, the ability to attach files, electronic signatures, and the ability to track progress notes, treatment plans, and assessments.
Click here for answers to your most frequently asked questions about EMR selection and transition.
In Touch EMR has grown to over 1000 clients, our company / founders have been mentioned on CNN, Forbes, Huffington Post, Amazon, been featured as a Cleardata success story, received the prestigious ONC certification, 2015 and 2016 PQRS registry designation, integrated with Microsoft’s cutting edge patient portal technology and initiated groundbreaking healthcare partnerships with companies like Novartis. All of this is possible thanks to clients across the country, who have embraced In Touch EMR.
In Touch EMR is featured on our HIPAA compliant hosting partner (Cleardata) website along with other industry leaders such as the Cleveland clinic, Nexttech, Saint Mary’s regional medical center and UCLA health.
 SIMPLE, TRANSPARENT PRICING MODEL
SIMPLE, TRANSPARENT PRICING MODEL
At In Touch EMR, we charge a flat fee per licensed clinician (no hidden fees or surprises) and it includes everything, unlimited claims and notes and infinite custom template creation. We are also a CMS recognized PQRS registry, we automate the reporting of PQRS and Functional Limitation G codes and provide automatic alerts for plan of care expirations, authorizations, progress note reminders and KX modifier alerts.
Clients also get a self-paced video training program on how to get up and running, custom documentation template builder, iPad app – one touch document import, Instant Intake iPad app, unlimited patient manager and patient portal.
Every license unlimited ongoing support (phone / email / live chat), billing software integration, unlimited appointments, unlimited documentation, unlimited document uploads and unlimited electronic faxing.
OFFICE OF THE NATIONAL COORDINATOR CERTIFIED ELECTRONIC HEALTH RECORD TECHNOLOGY
We are a premier vendor in the rehabilitation space, and on the prestigious, certified Health IT Product List, which is a division of the office of the National Coordinator for Health Information Technology, a division of the Department of Health and Human Services.
Very few vendors can make this claim, and they generally won’t bring this up (in some cases, out of ignorance) mostly because this is not a mandatory certification, it is optional and requires a significant investment of time and effort. This certification is a sign of our commitment to a HIPAA compliant, secure and stable EMR system for your clinic.
If you ever get audited, the fact that you are using ONC-certified EHR technology (CEHRT) will work in your favor. CMS looks favorably on the use of CEHRT since HHS is trying to encourage the adoption of CEHRT amongs providers nationwide as part of a long term push towards electronic documentation and interoperability between EMR systems. Your practice can state that it carefully vetted and selected “a rehabilitation-specific vendor that passed all of the ONC HIT 2014 Edition EHR Certification criteria required to satisfy the Base EHR definition”
Since In Touch EMR has been very proactive at staying at the forefront of emerging guidelines for EMR vendors, you are assured higher quality, higher security and more compliance with CMS and other payer regulations.
For more information about the ONC, please visit: http://www.healthit.gov/newsroom/about-onc
In Touch EMR is one of the only EMR vendors in the rehabilitation space to pass all the 2014 Edition EHR Certification criteria required to satisfy the Base EHR Definition as stated by the Office of the National Coordinator for Health Information Technology, as listed here:http://www.healthit.gov/sites/default/files/pdf/BaseEHR_8-18-12_Final.pdf
In Touch EMR is on the Certified Health IT Product List (CHPL) website.
http://www.healthit.gov/policy-researchers-implementers/certified-health-it-product-list-chpl
Search for In Touch EMR > CHPL Product Number: 150002R00
PRAISE FROM THOUSANDS OF SATISFIED CLINICS ACROSS THE UNITED STATES
“In Touch EMR has emerged as a comprehensive, customizable EMR solution for our growing organization. Support is always there when we need it, options to customize options to match our workflow are endless, clinicians find it simple and easy to use, front desk and billing love the integration between documentation and claims and compliance is built-in. This is exactly what we needed and it has boosted our efficiency. Couldn’t have asked for more. In Touch EMR is a leader in web-based EMR for our practice. Thank you!”
Julie Edelman PT, DPT – Avanti Therapy
“Moving to In Touch EMR was a process of adjustment, but it was worth it, for several reasons. Not only has the staff at In Touch EMR been proactive in adding new features and responding to support calls and streamlining our billing processes, they have been understanding, professional, polite and patient. The ability to create our own documentation templates, generate professional reports on demand and submit claims to billing with one click has allowed us to streamline our practice. The billing software is extremely versatile – I can review number of claims sent / on hold, payer breakdown, charges per visit and collections per visit. Our biller is able to pull up detailed reports, exactly the way we want. My front desk staff has the ability to track authorizations and create progress note alerts, physician prescription alerts and fax reports to physicians with the click of a button in In Touch EMR. My management is now exploring analytics to identify areas of growth and efficiency and expect to drive our practice further with analytic insights. Best of all, the transition for our entire staff was streamlined and consistent and help was readily available. I like that we are able to talk to someone whenever we need to. If you are looking for a powerful, reliable, and responsive team to help you implement EMR and billing software to grow your practice, look no further than the team at In Touch EMR. We support this therapist owned EMR company wholeheartedly.”
Matthew S. Fischer, MSPT – Fischer Physical Therapy
“In my 30+ years as a compliance auditor, author and instructor, I have yet to see an EMR and billing software as comprehensive as In Touch EMR. If you are looking for compliant ICD-10 documentation, and a ‘gold standard’ that can survive auditing, get In Touch EMR. A well defined workflow for the front desk, clinicians, billers and coders makes this a one-stop shop for quick, compliant documentation and flawless billing. I’m impressed with their HIPAA compliance, PHI protection and data breach prevention protocols. The front desk automation (certification alerts, patient portal, birthday reminders, e-newsletters) and clinician automation (progress note and reevaluation countdown, autotext technology, flowsheet templates, tasks and messages) are sufficient to set them apart. They didn’t stop there. The billing automation (claim cleanser, automatic transmission to billing, CCI edits – modifier 59 automation, autopost ERAs) and the administrator functions (access controls, audit logs, time tracking, productivity metrics) result in an incredible EMR and billing software combination for all clinicians. It’s a no brainer – forget the hype from other products and get In Touch EMR”
Cheryl House RMC, CHI Compliance Auditor, Author, Coder and Instructor at Illinois Valley Community College
“I was looking for a Practice Management Software that combined both documentation and billing platform systems that work in unison. I had previously tried more complicated systems that made me exhausted at the end of the day. In Touch EMR and In Touch Biller Pro represent a united and unified package that helps the private practice clinician govern a practice. It’s easy to use, it is concise, and it has a plenty of analysis variables to study.”
Sammy K. Bonfim PT – Rehabilitation & Performance Center
All In Touch EMR customers get unlimited support via phone, email and live chat.
Click below to schedule a free demo with the experts at In Touch EMR, or call (800)-421-8442 to learn more.
Schedule a Demo of In Touch EMR Now
At In Touch EMR, we charge a flat fee per licensed clinician (no hidden fees or surprises) and it includes everything, unlimited claims and notes and infinite custom template creation. Schedule a demo to see why practices across the country are switching to In Touch EMR.